 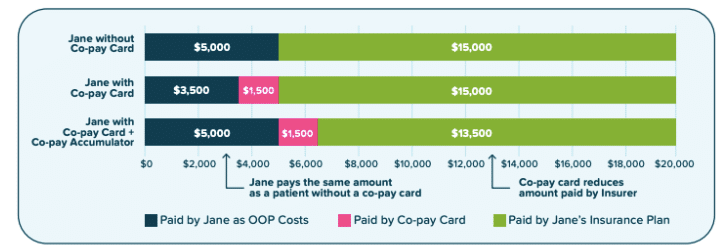
"Cost-sharing requirement" is defined as any copayment, coinsurance, deductible, or annual limitation on cost-sharing required in order to receive health care services, including prescription drugs. Requires health insurance carriers and pharmacy benefits managers to include cost-sharing contributions paid by or on behalf of the enrollee when calculating any enrollee cost-sharing requirement. Requires health carriers, pharmacy benefit managers, and managed care organizations to count any discounts or payment made by a third party on behalf of a plan enrollee toward the enrollee’s coinsurance, copayment, deductible, and other out-of-pocket expenses for a covered prescription drug benefit. Excludes cost-sharing for a brand drug if the brand drug is A.) not considered to be medically necessary by the prescriber and B.) has a medically appropriate generic equivalent. Requires any cost-sharing paid by or on behalf of the enrollee to count toward the enrollee’s applicable cost-sharing requirement. 
Requires health insurers and pharmacy benefit managers to count the value of contributions made by or on behalf of enrollees toward enrollees’ cost-sharing requirements (e.g., out-of-pocket maximum, deductible, copayment, coinsurance) for prescription drugs that either 1) do not have generic equivalents or 2) do have generic equivalents, but the enrollee obtained access to the prescription drug through: Prior authorization Step therapy or The health insurer’s exceptions and appeals process. Has Laws Limiting Co-Pay Accumulator Programs Link Has Laws Limiting Co-Pay Accumulator Programs
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
